
Beginning July 1, 2019, there will be a new health plan in place for employees who are enrolled in BlueCross BlueShield (BCBS) or UNM Team Health (UNMTH).
In order to provide a simplified and financially predictable medical benefit structure, UNM is combining the current UNMTH and BCBS medical insurance plans into one new plan – UNM LoboHealth.
The new plan – UNM LoboHealth – will reduce administrative redundancy and continue to provide UNM employees and dependents with expanded health care choices. UNM LoboHealth will also increase utilization of the Tier 1 network and provide a framework for more sustainable benefits into the future. (Translation: there will be more providers available in the network, enhanced customer service, and lower out-of-pocket expenses!)
The Presbyterian Health Plan will remain the same.
The following comparison and examples describe what the costs and services will look like when the populations of the BCBS and UNMTH plans are combined.
The UNM LoboHealth plan was developed by Benefits and approved by the various groups represented below. BlueCross BlueShield and UNM Team Health plan participants will automatically be enrolled in UNM LoboHealth effective July 1, 2019, unless they elect the Presbyterian Health Plan during Open Enrollment. Open Enrollment for health, life, and disability insurance benefits is tentatively scheduled to take place April 24 – May 10, 2019.
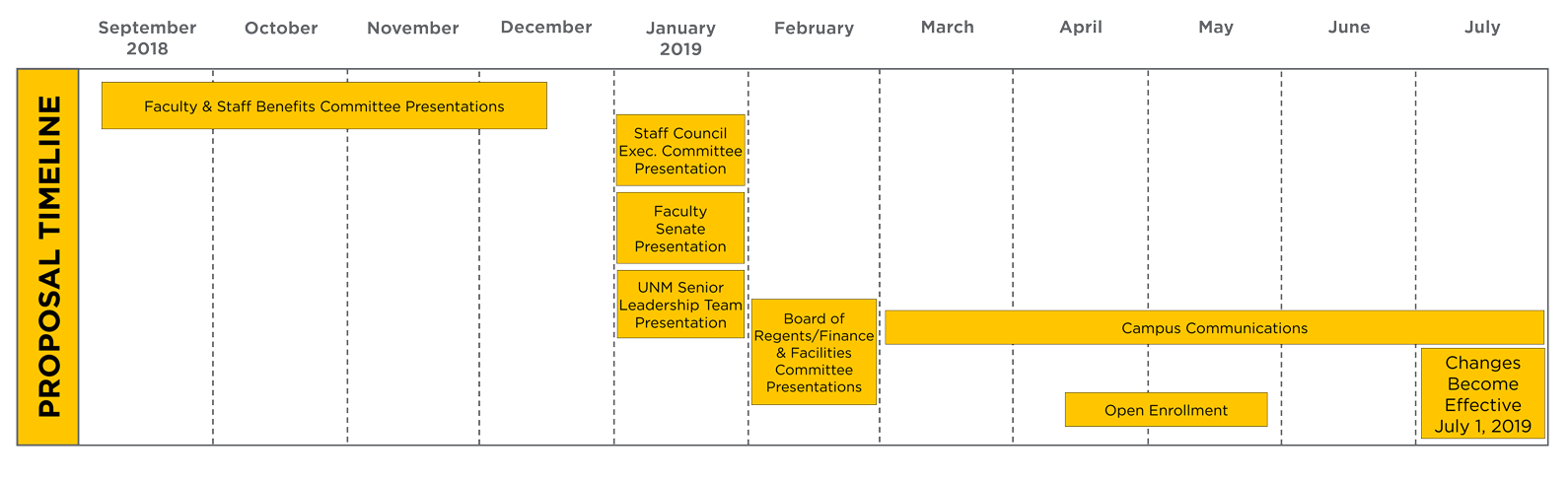 Click to Enlarge
Click to Enlarge
For questions regarding this change, contact the Human Resources Service Center at (505) 277-6947 or a Benefits representative via email at hrbenefits@unm.edu.